A Smithsonian magazine special report
Can Smartwatches Be Adapted to Help Detect Covid-19 Infections?
With new algorithms, wearable devices—collecting vital signs like heart rate and skin temperature—could catch illness early
/https://tf-cmsv2-smithsonianmag-media.s3.amazonaws.com/filer/16/59/165987da-c8d6-49f9-b823-6dbd1b73e02c/wearables-covid-1600x600.gif)
Five years ago, on a flight to Norway, Stanford University biologist Michael Snyder noticed that his body wasn’t behaving as it should. According to the multiple fitness trackers he happened to be wearing at the time, his heart rate was unusually high and his pulse ox — a measure of blood oxygen level — was unusually low. “When I landed, they never came back to normal,” he says. “So I knew something was up.”
Snyder could guess what that something was: Two weeks earlier, he’d helped his brother install a fence in rural Massachusetts — tick country. Sure enough, soon after landing in Norway, he developed a fever consistent with Lyme disease. A Norwegian doctor gave him antibiotics to fight the infection until he returned home, when a test confirmed the diagnosis. “And the first clues were actually from my smartwatch and pulse ox,” Snyder says. “Pretty cool.”
Snyder was wearing the devices as part of an ongoing study, started in 2010, in which his lab is tracking wearable and other data from about a hundred people, including him. (As we speak, he flashes his wrists, brandishing no fewer than four smartwatches.) “At the time we started, most people weren’t really even using them for health purposes,” he says — just to monitor daily activity. “We realized, Gosh, these are pretty good 24-7 monitors of your physiology.” He wondered what one could learn from all those data.
Maybe a lot. In a review of Snyder’s personal smartwatch data over the two years before his Lyme disease experience, his team found evidence for three viral infections that had already been confirmed by testing — including one that was asymptomatic. “So every time I was ill, we could pick it up with high heart rate and skin temperature — prior to symptom onset,” he says. The researchers began to design algorithms to identify deviations from baseline vitals in anyone, with the goal of combining genetic, wearable and other data to predict metabolic disorders, estimate cardiovascular risk and make other health assessments remotely.
Thus began a research path — now joined by labs around the world — that could enable smartwatches to detect when people are infected with Covid-19 before they’re tested, or even before they feel sick. In recent years, Snyder and a number of other research groups have used wearable devices to monitor heart health and detect infectious disease. Now, many have hope that the gadgets can be leveraged in the battle to stop the spread of Covid-19.
All in the wrist
SARS-CoV-2, the virus that causes Covid-19, has infected more than 100 million people and killed more than 2 million. Accelerating its spread, people carrying the virus can transmit it to others without knowing they’re infected. Massive rapid testing could curtail such transmission by alerting people to the infection, but most people don’t get tested every day, and there wouldn’t be sufficient resources to do so anyway. Finding ways to quickly identify those most likely to test positive could save lives.
As Snyder suggests, the appeal of using smartwatches, fitness trackers and other such gadgets for this purpose is that they can monitor (depending on the device) heart rate, breathing rate, sleep, temperature, blood pressure and activity levels — and that tens of millions of Americans are already wearing them.
“We see a potential to help” with Covid-19, says Giorgio Quer, the director of artificial intelligence at Scripps Research Translational Institute and one of the leaders of DETECT, one of the largest efforts so far to test this idea.
In October, his team published a paper in Nature Medicine reporting on their findings in a study of 30,000 people who shared their health data last spring. They focused on device users who had been tested for Covid-19 at least once and who’d reported symptoms or lack thereof on a custom smartphone app.
The study used a common accuracy metric called AUC; a high AUC requires minimizing both false positives and false negatives. The researchers’ primary question was whether wearable information — resting heart rate, sleep and activity — would add anything to self-reported symptoms. Indeed, it did. Using only symptoms, the simple hand-coded algorithm scored an AUC of 0.71. Daily sensor data alone performed about the same — 0.72. But by adding sensors to symptoms, the AUC reached 0.80, a statistically significant improvement. “The findings there are really exciting,” Quer says.
In November, Snyder’s team at Stanford published a paper in Nature Biomedical Engineering describing their study of about 5,000 participants. It differs from the Scripps study in its resolution, zooming in on hour-by-hour changes in some measures. The Stanford group’s algorithm collects data on three signals, all relative to the person’s baseline — a high resting heart rate (a result of inflammation), a high ratio of resting heart rate to daily steps taken, and increased sleep (one way the body activates immune cells) — and looks for trends. Among 32 device wearers who had experienced Covid-19 symptoms, it detected signals related to reported symptoms a median of four days before those symptoms appeared.
One limitation, though, is that this analysis, like the one at Scripps, was retrospective. That is, it looked back at data collected both before and after a prediction point, which isn’t much use if you want to catch infection as it happens. The eventual goal is a prospective system that detects possible illness in real time, helping wearers decide whether to seek testing or self-isolate.
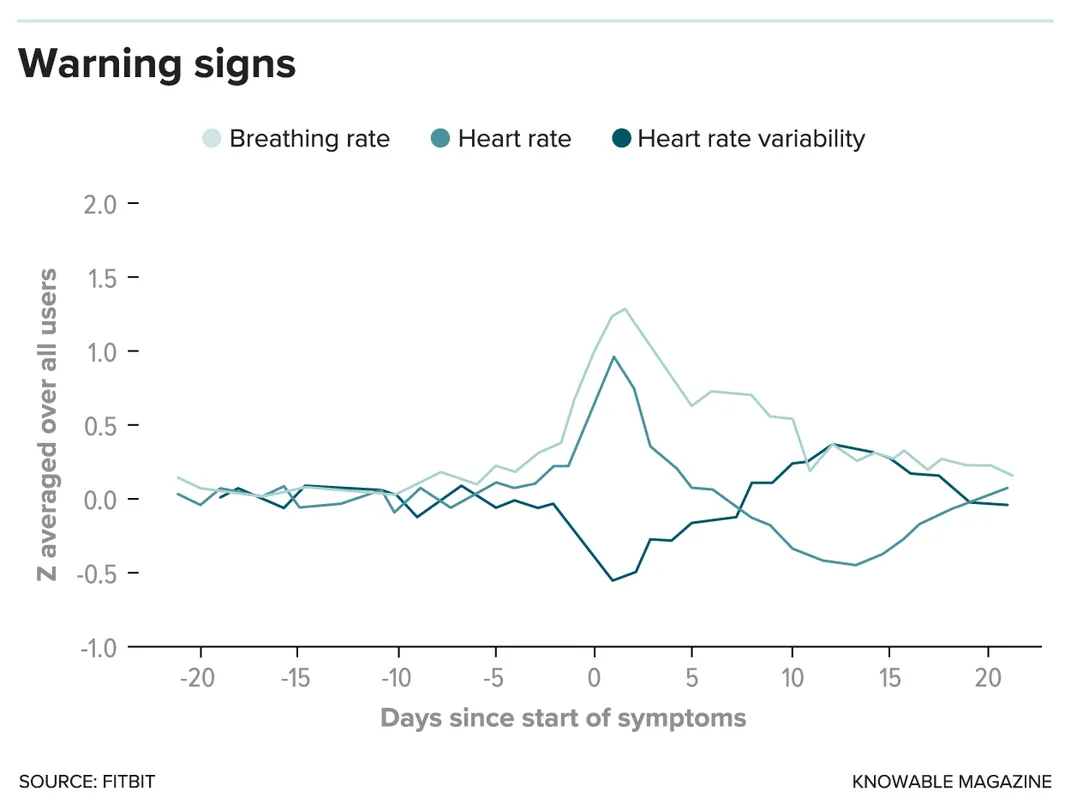
Snyder’s team did also evaluate their system in prospective mode. They ran a simulation: At any given point, if they ignored data they had collected after that point, could their system detect illness, even if there had been no reported symptoms? Twenty-four Fitbit wearers who’d gotten sick had enough presymptomatic data to test this hypothesis. In 15 of them, the system caught the illness.
Stanford is now piloting a system that alerts wearable-device users to possible Covid-19 infection, using a two-alarm system. If signals surpass a certain threshold, it produces a yellow alarm. If they remain elevated for 12 hours, it produces a red alarm, strongly suggesting testing or isolating. If there were only a yellow alarm, Snyder says, frequent false alarms might cause some people to ignore alarms completely. Their system has already detected several cases in which the alarm has gone off prior to symptom onset, and it works with several watch types.
Scripps is also designing an alert system, Quer says. Such systems don’t require FDA approval as long as they don’t offer diagnoses, he says. They might simply say you have an elevated heartrate, which correlates with various issues, including a respiratory virus such as Covid-19 or the flu. “It’s kind of like your thermometer,” Snyder says. “An elevated temperature could be due to several things.”
Challenges
One of the key challenges in any such alert system is the amount of uncertainty in the signal, making it hard to establish crisp baselines that, when breached, indicate a possible problem. Some people, for example, are on medications that muddy the data by affecting heart rate, or they have difficulty breathing due to severe asthma, as some did in Snyder’s study. And alarms can also be triggered by factors other than infection, including long flights, alcohol or stress. (“We call it the holiday bump,” Snyder says, whether due to travel or drinking or in-laws.)
Researchers at Purdue University and a health technology company called physIQ are trying to meet this challenge in a study to improve wearable signals, with an eye toward Covid-19 detection. Participants wear a Samsung smartwatch and an electrocardiogram patch on their chest for five days. The patch collects more reliable heart rate data than the watch does. The researchers use it as training data so an algorithm can learn to interpret the watch data in a way that aligns with the patch data. Their goal is “to figure out how to get as much out of the wrist device as possible,” says Stephan Wegerich, physIQ’s chief science officer.
The study also examines usability. Participants must wear the watch snugly to improve the signals, and, unlike with factory settings, it collects raw data at a high frequency, so users have to charge it twice a day for several hours to keep the battery alive. While that could make some casual smartwatch wearers balk, so far study participants haven’t complained. Craig Goergen, a bioengineer at Purdue, says it’s not been difficult for participants to figure out a routine that works for them. Worry over Covid-19 may motivate many more.
One limitation to existing studies is that participants might be representative of smartwatch owners who are conscious of Covid-19 infection, but not representative of the wider population. Duke University’s CovIdentify project aims to ameliorate that problem. As in several other studies, anyone with a smartwatch can enroll, but, according to Jessilyn Dunn, a biomedical engineer at Duke, they’ve also given out 400 devices to those who didn’t have them. They’ve yet to report results.
Meanwhile, Fitbit has conducted its own study, published in November in npj Digital Medicine. Their neural network, when limited to a false positive rate of 5 percent (the setting is adjustable), could detect 15 percent of Covid cases, and do so a day before onset of symptoms, using data from that day and the previous four. Not great, but better than nothing. Fitbit recently received $2.5 million from the Army to provide thousands of devices to healthcare workers and test a notification system for use in the field.
But if you build it, will they come? “Even if these technologies exist, just having the technology alone is usually not enough,” says physician Mitesh Patel, director of the Penn Medicine Nudge Unit and coauthor of a paper in the Annual Review of Medicine on using wearable devices to monitor cardiovascular disease. “You might get the young and engaged, the quantified-selfers, to use these devices for Covid detection or heart rate variability,” he says. “But to get older patients, or the unmotivated, or patients of lower socioeconomic status, we have to think about mechanisms to both provide access and increase engagement.”
Engagement is especially urgent, he says, because those are the groups that could benefit most from these types of algorithms. Behavioral nudges to encourage usage might include having families use them as a group, or having employers offer monetary incentives.
Patel and others say they’re encouraged by recent progress, and that wearables may eventually be used to inform clinical decisions, beyond everyday wellness applications. According to Snyder, what they’re learning about Covid-19 detection might be applied to future pandemics, seasonal flu and other areas of medicine and public health. It could potentially save many lives. “The pandemic has really brought all of that to a head,” says Dunn, of Duke. “So I’m excited for us to be able to demonstrate what these things can do.”


