How a Mother’s Depression Shows Up in Her Baby’s DNA
Researchers find that at just 18 months, infants can have cellular damage related to stress
/https://tf-cmsv2-smithsonianmag-media.s3.amazonaws.com/filer/40/41/404170b6-62e7-43ff-b501-7cee8d9074ee/file-20180116-53307-epjvhk.jpg)
An estimated 1 in 9 women experience symptoms of postpartum depression. These symptoms – including mood swings, fatigue and reduced interest in activities – can make it difficult for mothers to bond with their newborns.
Early relationships between mothers and their infants can influence health across the lifespan, for better or worse. For example, adults who report more household dysfunction and abuse during their childhood are more likely to suffer disease as adults. Those with healthy and supportive relationships during early life are better at handling stress and regulating their emotions.
However, scientists do not completely understand how these environments get “under the skin” to shape health. Our latest paper, published in November, shows a possible link between increasing depression symptoms in mothers and cellular damage in their infants.
Telomeres and health
How does stress affect our cells? One area of burgeoning research focuses on telomeres.
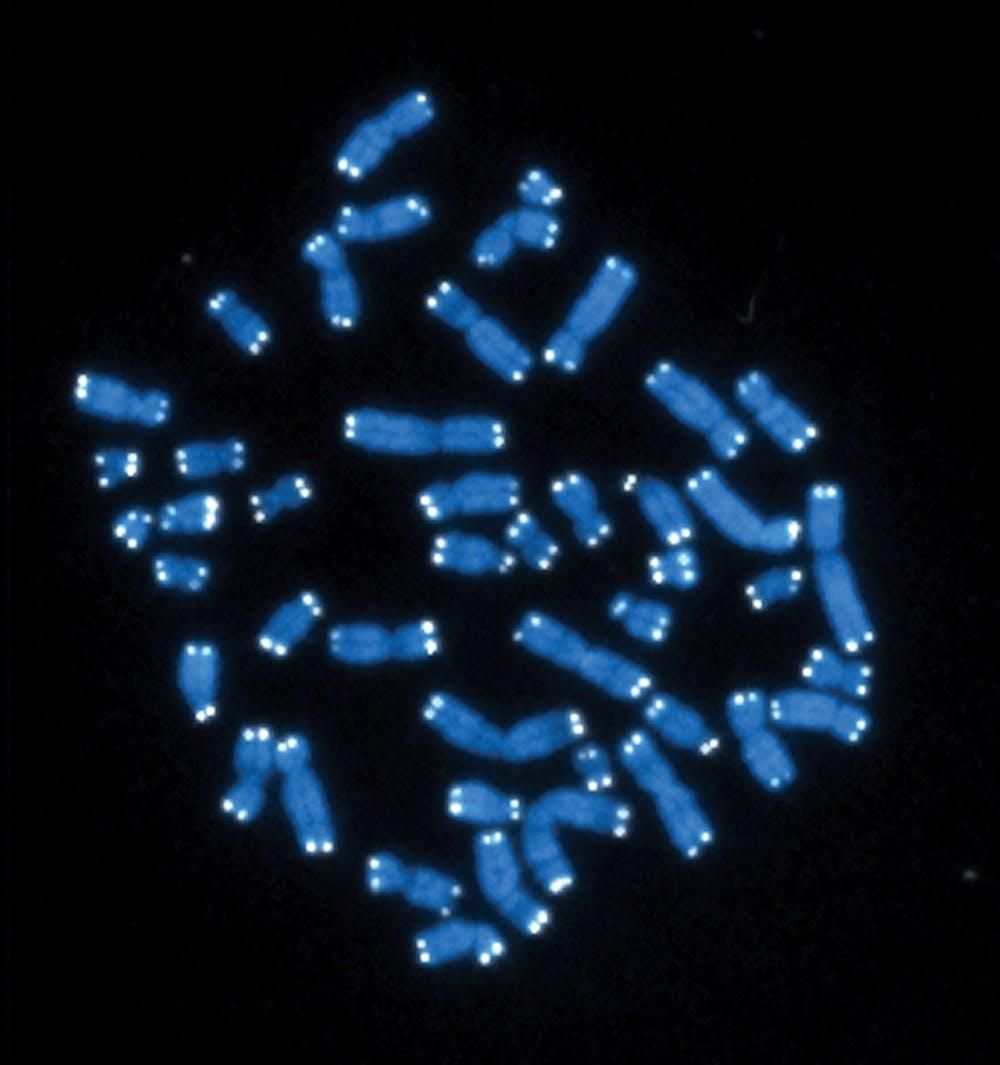
Telomeres are caps at the end of our DNA that protect chromosomes. They’re analogous to the plastic tips at the end of shoelaces that keep laces from unraveling. In essence, these plastic caps keep laces functional. The same can be said of your telomeres.
Since the length of telomeres is affected by our genetics and age, they’re sometimes thought of as part of a “biological clock” that reflects the age of our cells. As telomeres shorten over time, people are more likely to experience a host of negative health outcomes, such as cardiovascular disease, dementia, diabetes, cancer, obesity and even death.
Interestingly, telomeres can degrade more quickly when a person suffers from psychological stress. When we experience stress, our bodies release a hormone called cortisol, which influences our emotional responses as well as our energy metabolism, learning and memory. This may be one mechanism that connects psychological stress to telomere length and ultimately physical health. Cells that are exposed to cortisol have shorter telomeres and less telomerase, which is the enzyme responsible for maintaining the ends of telomeres.
This process may explain how psychological stress is converted to biological “wear and tear.” Indeed, adolescents with depressed mothers have heightened cortisol stress responses and shorter telomeres than their peers, even when the adolescents themselves are not depressed.
Our study
We examined whether increasing maternal depressive symptoms affected infant stress and later cell health.
Infancy is a sensitive period, when individuals are strongly influenced by their environment. One way to study how early stress may influence health is to look at how infants respond to their parents’ stress. Studies suggest that infants exposed to maternal depression may be less likely to engage socially and experience more negative emotion.
For our study we recruited 48 mothers with 12-week-old infants and followed these families until the infants were 18 months old. At 6 and 12 months of age, the infants were brought to the lab to engage in mildly stressful tasks. For example, in the “still face experiment,” mothers alternated between playing with their infant and not reacting to their infant’s bids for attention. This can elicit stress in infants, as they rely on their caregivers to not only feed them, but to also soothe their emotions.
During each visit, we measured infants’ stress by collecting saliva samples to look at changes in cortisol. We also collected information on how many depression symptoms mothers were feeling. Finally, when the infants were 18 months of age, we brought the families back into our lab and collected saliva to measure the length of the infant’s telomeres.
Worsening depression symptoms in mothers related to greater infant cortisol stress responses between 6 and 12 months of age. In addition, infants with higher cortisol stress responses were more likely to have shorter telomeres at 18 months of age, indicating greater cellular wear and tear.
Better mental health
While these findings are preliminary and should be replicated with a larger group of infants, our results highlight how patterns of health across the lifespan may be influenced in the first 18 months of life. This early stress may put young children on track for the early onset of poor health outcomes.
The silver lining is that infancy is a sensitive developmental period, when humans are especially responsive to their environments. Fostering positive experiences between infants and their mothers – as well as providing affordable, scientifically supported treatment services for mothers experiencing depression – may allow infants to move toward a healthier life trajectory.
In our view, these results show how important it is to fund effective maternal mental health treatment and early childhood policies.
This article was originally published on The Conversation.
Benjamin W. Nelson, Doctoral Student in Clinical Psychology, University of Oregon
Heidemarie Laurent, Assistant Professor of Psychology, University of Illinois at Urbana-Champaign
Nick Allen, Ann Swindells Professor of Clinical Psychology, University of Oregon

