Discovered: A Natural Protein in Breast Milk That Fights HIV
Scientists have identified a milk protein called Tenascin C that binds to HIV and prevents it from injecting its DNA into human cells
/https://tf-cmsv2-smithsonianmag-media.s3.amazonaws.com/filer/Surprising-SCience-breast-milk-HIV-prevent.jpg)
For decades, public health officials have puzzled over a surprising fact about HIV: Only about 10-20 percent of infants who are breastfed by infected mothers catch the virus. Tests show, though, that HIV is indeed present in breast milk, so these children are exposed to the virus multiple times daily for the first several months (or even years) of their lives.
Now, a group of scientists and doctors from Duke University has figured out why these babies don’t get infected. Human breast milk naturally contains a protein called Tenascin C that neutralizes HIV and, in most cases, prevents it from being passed from mother to child. Eventually, they say, the protein could potentially be valuable as an HIV-fighting tool for both infants and adults that are either HIV-positive or at risk of contracting the infection.
The research, published today in Proceedings of the National Academy of Sciences, was inspired by previous work by other researchers showing that, both in tissue cultures and live mice, breast milk from HIV-negative mothers was naturally endowed with HIV-fighting properties. Scientists suggested that a few different proteins in the milk could potentially be responsible, but no one knew which one.
As part of the study, the researchers divided breast milk into smaller fractions made up of specific proteins via a number of filters—separating the proteins by size, electrical charge and other characteristics—and tested which of these fractions, when added to a tissue culture, prevented the cells from being infected by HIV. Eventually, using mass spectrometry, they found that one particular protein was present in all the HIV-resistant fractions but in none of the others: Tenascin C.
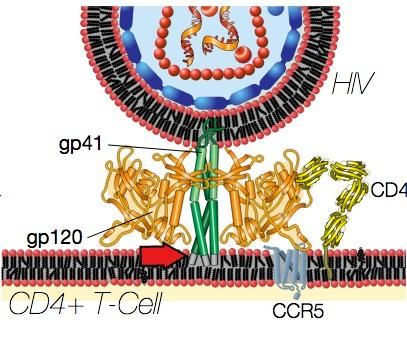
“The protein works by binding to the HIV envelope, and one of the interesting things is that we were even able to narrow down exactly where on the envelope it binds,” says Sallie Permar, the study’s lead author. Her team found that the protein binds to a crucial region on the virus’ envelope that normally locks onto a receptor called CCR5 on the outside of human T cells,allowing it to fuse its membrane with the cell’s. With the region covered up by Tenascin C, HIV’s normal route of attack is blocked, and the virus’ effectiveness is greatly diminished.
Still, the researchers say that other natural elements in milk might play a role in fighting HIV as well. “It’s clearly not the whole story, because we do have samples that have low amounts of this protein but still have HIV-neutralizing activity,” Permar says. ”So it may be acting in concert with other antiviral and antimicrobial factors in the milk.”
Whatever those other factors are, though, the finding vindicates recent changes to UN guidelines that recommend even HIV-positive mothers in resource-poor countries should breastfeed, if they’re taking anti-retroviral drugs to combat their own infection. That’s because—as statistics bear out—the immense nutritional and immune system-boosting benefits of breast milk outweigh the relatively small chance of transmitting HIV through breastfeeding. Tenascin C, it seems, is a big part of why that transmission rate is surprisingly low, and sufficient access to anti-retroviral drugs can help drive it even lower—as low as 2 percent.
The next steps, Permar says, are determining which area of Tenascin C is active in binding to HIV and whether it can effectively prevent transmission in a live animal, as opposed to a tissue culture. If it works, it could potentially be incorporated into an HIV drug with broader applications. Possible uses include giving it in a concentrated form to infants who can’t breastfeed or even administering it to those who do to increase their level or resistance. It’s even conceivable that it could someday be adapted to reduce the risk of HIV transmission in adults as well.
One immediate advantage, says Permar, is that “it’s like to be inherently safe, because it’s already a component for breast milk. It’s something babies eat everyday.” Other potential treatments, on the other hand, must be screened for toxicity.
Tenascin C’s presence in breast milk, though, prompts a deeper question: Why would milk naturally include a protein that battles HIV, a virus that evolved extremely recently in our evolutionary history, sometime in the early 20th century?
“I don’t think it’s in breast milk to combat HIV specifically, but there have been other, related infections that have passed through breastfeeding,” Permar says. “Our work has shown that Tenascin C’s activity isn’t specific to HIV, so we think it’s more of a broad-spectrum anti-microbial protein.”
In other words, Tenascin C is effective at combating a large variety of infections (perhaps related to its role in adults, where it holds various types of tissue together, necessitating receptors that can bind to a wide array of different cells). The fact that it happens to bind at just the right spot on HIV’s outer envelope so that it combats the virus’ transmission, as Permar puts it, is “a gift from evolution.”
/https://tf-cmsv2-smithsonianmag-media.s3.amazonaws.com/accounts/headshot/joseph-stromberg-240.jpg)
/https://tf-cmsv2-smithsonianmag-media.s3.amazonaws.com/accounts/headshot/joseph-stromberg-240.jpg)