A Microwave Helmet May Help Diagnose Traumatic Brain Injury
Doctors find that a stroke-detection technology could be useful in screening for intracranial bleeding
/https://tf-cmsv2-smithsonianmag-media.s3.amazonaws.com/filer/55/7f/557f7f16-c922-4d76-91ae-17e44d417f16/hematoma.jpg)
Whether from sports, car crashes or military service, traumatic brain injuries are prevalent and dangerous. According to the Centers for Disease Control and Prevention, 30 percent of deaths due to injury feature TBIs. In 2013, that amounted to nearly 50,000 deaths in the United States.
Some TBIs, especially the more severe ones, are characterized by bleeding in the brain (intracranial), and these require a different kind of treatment, where the skull is opened to release pressure and remove the clotted blood, called a hematoma. Sending people with those injuries to the appropriate neurotrauma centers is a matter of life or death; the survival rate for patients with intracranial bleeding due to TBI drops from 70 percent to 10 percent if the hematoma is not removed within four hours, according to a 1981 study in the New England Journal of Medicine.
But concussion diagnosis is inexact, and in the case of hematomas, requires a CT scan, which is expensive, and often has a long queue. A brainstorm from researchers at the Chalmers University of Technology in Sweden led to an article, published in the Journal of Neurotrauma, assessing a new use of a stroke-detecting technology to quickly diagnose intracranial bleeding.
“That is in many areas a big problem that we need to address, because it is difficult to sort the right people to come to neurosurgery,” says Johan Ljungqvist, the lead researcher, and a neurosurgeon at Sahlgrenska University Hospital.
Ljungqvist and his team conceived an off-label use for a pre-existing technology. The Strokefinder, built by Medfield Diagnostics, is a tool used to discern between ischemic strokes (those where a clot blocks the blood flow) and hemorrhagic ones (which involve bleeding). The helmet has eight microwave antennas on it. Each antenna fires, in turn, a small amount of microwave radiation through the brain (between 1/100th and 1/10th what you receive from a cell phone conversation) and the other antennas pick it up. The process is repeated at several different frequencies. The microwaves will have progressed through the tissue in different ways, depending on the consistency of the tissue, and when filtered via an algorithm, the hematoma stands out, whether it’s due to a stroke or a TBI.
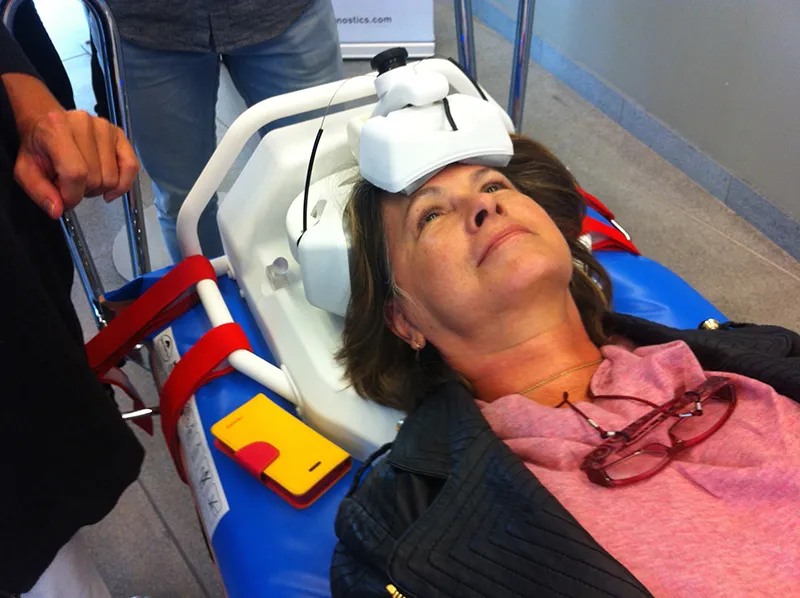
Doctors can immediately begin to treat stroke patients who are evaluated with the Strokefinder, but in the case of TBIs the usefulness is in taking them to hospitals prepared to give them the neurological care they need.
“It’s not so much an issue of being able to do more for them [TBI patients] pre-hospital wise, it’s a question of triage, of transporting them to the right hospital, and that’s a huge problem,” says Mikal Elam, chair of clinical neurophysiology at the University of Gothenburg, and one of Ljungqvist’s co-researchers.
So far, the technique has been applied only to people with chronic brain hematoma—non-life threatening versions that don’t require immediate surgery. But based on the success of this study, Ljungqvist thinks using it in urgent situations will be feasible.
“If we can prove that it works for these [chronic] hematomas, then we can proceed to try other patients as well, with acute hematomas, and they have different dielectric properties that could actually be easier to find. In that case, we could have this as a screening instrument in ambulances or helicopters,” he says.
It could even appear in stadiums and at sporting events or on battlefields. Though the device is currently only available to researchers, Medfield has plans to make it available commercially, and with that scale, the price will come down (though at around $100,000 it’s already far less than a CT machine).

Medfield is collaborating with Chalmers and Gothenburg’s Sahlgrenska University Hospital on projects featuring the Strokefinder and other technologies, figuring the doctors and medical researchers there will have a better idea what they need than the engineers at the company. “As an engineering school, you might have ideas, but it’s really their profession, it’s up to the medical community to decide how to use this,” says Mikael Persson, who founded Medfield after Elam’s lab showed that an early prototype could detect changes to the tissue in the brain.
The device itself is quiet, and shaped sort of like a chunky helmet, with paddles over four sides of the head. It weighs a little more than 10 pounds. You can’t feel it working. The algorithm differentiates between normal tissue and clotted blood, and the whole process takes just 45 seconds. It doesn’t provide an image, merely an indication whether a hematoma is present.
Microwave refraction has been used to detect breast cancers, and Elam and Ljungqvist think it could be applied in still more areas. A group in Norway is using the technology to diagnose collapsed lungs in pigs, and in the future it may get used for other types of brain swelling or abdominal bleeding. Ljungqvist is planning a study in patients with acute TBI-caused hematoma, because the process is fast enough that it needn’t delay surgery or CT scans.
As these and other studies progress, the device’s algorithm will get refined to provide more detail, like size and location of hematoma, says Elam.
“This is not an imaging tool. It gives us a value, and that value is different from what normal people have without bleeding,” says Ljungqvist. “Since we don’t have any possibilities for imaging, we really need to find things that this algorithm can be used for.”