Anthony Fauci Is Waging War Against Zika, and Preparing for Other Epidemics to Come
The director of the National Institute of Allergy and Infectious Diseases talks about developing a Zika vaccine
:focal(365x190:366x191)/https://tf-cmsv2-smithsonianmag-media.s3.amazonaws.com/filer/0f/69/0f697fb1-7b2c-4523-89c1-994199ef3ffd/anthony-fauci.jpg)
It is one thing to know the science of epidemics—why they start, how they spread, who’s at risk. But to truly understand a disease’s impact, Anthony Fauci believes you need to see its victims. And so, last year, when a health care worker who had contracted Ebola in Sierra Leone was being treated at the National Institutes of Health, Fauci often broke from his busy schedule and donned a bulky protective suit so he could personally examine the patient.
That’s all part of the job for Fauci, who has been America’s point person in confronting epidemics and other public health crises for decades.
As director of the National Institute of Allergy and Infectious Diseases since 1984, he is the person who oversees the government’s research into outbreaks of infectious diseases, most recently the Zika virus and Ebola. He has been a leader in the fight again AIDS and HIV, and he also is one of America’s top advisors on bioterrorism. Among his numerous awards is the Presidential Medal of Freedom, the highest honor that can be given to a citizen by the president of the United States.
Smithsonian.com contributor Randy Rieland interviewed Fauci in advance of his appearance at Smithsonian magazine’s "Future Is Here" festival this weekend. He discussed the spread of the Zika virus, its unexpected consequences and how to prevent catastrophic epidemics in the modern world.
When do you think clinical trials for a Zika virus vaccine can begin?
I’m pretty sure we’ll be able to start phase one trials—at least to ask “Is it safe, and does it induce the kind of response you would predict might be protective?”—in September. But that’s just the first phase in a number of phases you need to go through in order to develop vaccines.
So when do you think a vaccine could be available?
It really is impossible to predict, because to be available it has to be shown to be effective. What will happen in early 2017 is that we likely will go into expanded efficacy trials, and if the vaccine is very effective, you’ll find that out sooner than later. The second factor is how many infections are occurring in the community. If there are a lot of infections, then the vaccine trial moves expeditiously and you can get an answer within a year. If the infections slow down, then it may take a few years to get an answer. Once you get an answer, you have to submit the data to the FDA for them to determine whether you can make it available to the public. It’s very difficult to put a time frame on it.
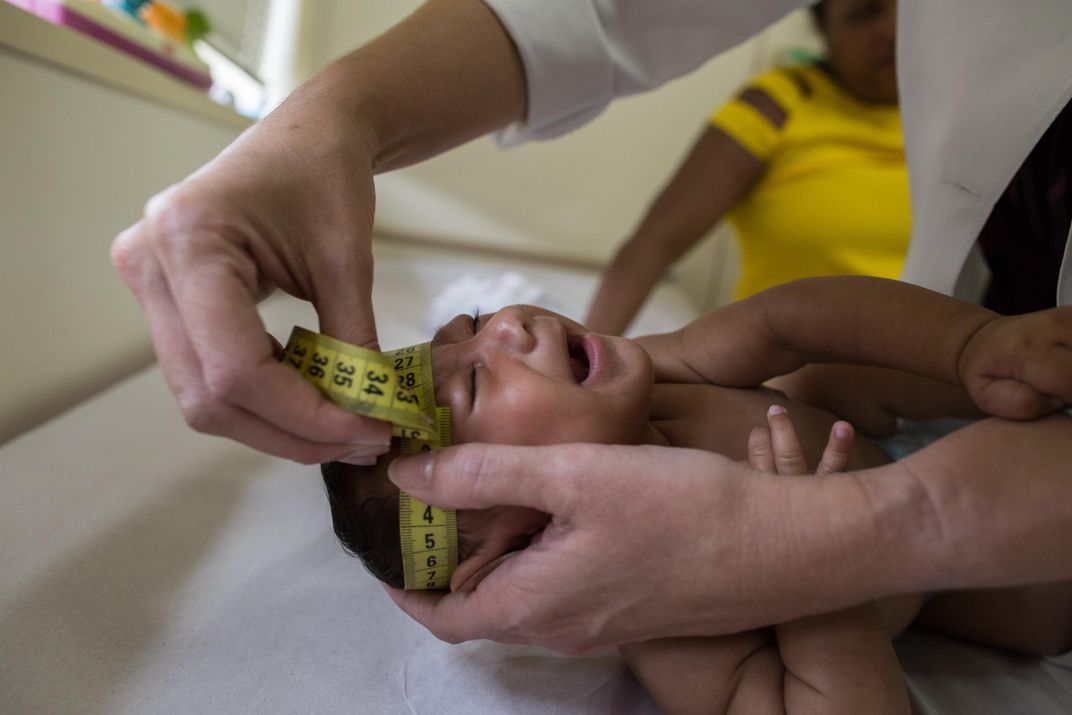
At one point, you were quoted as saying about Zika, “The more we know about this, the worse things seem to get.” What has been the most unsettling aspect of the spread of this virus?
The thing that has been most unsettling is the degree and frequency of the congenital abnormalities that we are seeing in women who are infected with Zika during pregnancy. Generally, these abnormalities have occurred when women are infected in the first trimester of their pregnancies. But now we’re finding that there are even deleterious effects on the fetus when the woman is infected during the second and even the third trimester. So that’s very disturbing that the vulnerability essentially lasts throughout the entire pregnancy.
The second thing is the high percentage of women who, when they are infected during pregnancy, are showing abnormalities in their fetus. We don’t know exactly what that number is, but the most accurate studies so far show that it’s at least 29 percent with gross abnormalities—there’s a much higher percentage of subtle abnormalities that you don’t notice until the baby is born and has difficulty at developmental landmarks, such as with hearing, with seeing, with intellectual capabilities.
So, it doesn’t look very good from the standpoint of the percentage of women who do get abnormalities with the fetus. That makes it more compelling for us to protect pregnant women and keep them away from the regions of the world where there is Zika, and if they live there, try and protect them as best as we can by mosquito control. It’s a very serious situation.
What do you think is the most critical information that people should know?
I get asked all the time by women who are pregnant, or thinking about getting pregnant, whether I’m sure they shouldn’t be going down to Brazil or other regions where Zika has spread. Absolutely, I’m sure. If you are pregnant or might be pregnant or are thinking about getting pregnant, you should not travel to a region where there’s a considerable degree of Zika. Also, if you’re a male and you go and travel to that region, and even if you don’t think you got infected—many of the infections are without symptoms—and you come back here to the United States, and you have a pregnant wife or a pregnant girlfriend, you need to make sure you use a condom consistently throughout the entire pregnancy. If you have a pregnant partner, you should make sure that at least for a period of eight weeks that you do not have unprotected sex.
Do you think the notion that there may have been an overreaction to the threat of the Ebola virus has affected how people have responded to the Zika outbreak?
No, I think the response has been appropriate. I certainly think the press has handled it really well. They’re covering it in an intellectually sound way. They’re not panicking. They’re reporting the truth—there is a real problem in South America, the Caribbean and Central America. We will almost certainly get a small degree of local outbreaks here in the United States. Hopefully, we’ll be able to contain them the same way we were able to contain local outbreaks of dengue fever and chikungunya in Florida and Texas. The real critical issue is how well we respond to that and prevent it from becoming a sustained outbreak.

It’s generally acknowledged that air travel has made controlling epidemics in the modern world more difficult. What else makes fighting epidemics more challenging today?
One of the things you have to do is recognize them as early as you possibly can so you can respond to them effectively. The United States has been an important part of that in setting a global health security agenda—to have communication and surveillance throughout the world, so if you do have an outbreak, you are able to recognize it and respond as early as you possibly can. We have been on top of things in regard to Zika because Brazil has a pretty good health care system and they were able to detect this early on. That was not the case in West Africa with Ebola. The first cases occurred in December of 2013, but it wasn’t until well into 2014 that anyone realized that there was a serious problem. So having good dissemination of information is one of the best things we can do to respond to these kinds of outbreaks.
Why do mosquito-borne illnesses tend to occur in waves?
Many of them are seasonal, and mosquitoes bite so widely that they infect a certain percentage of the population—almost all the vulnerable ones—and then it dies down for a bit until there’s a new cohort of susceptible people. So, it’s a combination of variations in weather and the climate depending on where you are. Even countries that are near the equator have seasons that are more or less amenable to mosquitoes. In Brazil right now, it’s just the end of their summer and they had a lot of mosquitoes during this past summer. But we hope, because of the Olympics in Brazil later this year, that by the time we get to our summer and their winter, the mosquito population will be lower there.
Can people, once they’re bitten, build up immunity to Zika?
We are not sure. But if Zika acts like dengue and West Nile virus acts, when you do get infected, you build up a certain amount of immunity that would likely protect you against a subsequent infection if you’re dealing with the same strain of Zika. Right now, it does not look like there are multiple strains of Zika. What we’re seeing in South America, the Caribbean and Central America is very closely related to the Asian strain from where we think it came. We believe the Zika came across the Pacific from Southeast Asia to Micronesia, French Polynesia and then South America.
How high would you say is the risk of Zika spreading in the southern U.S. this summer?
I think it is likely we’ll have a local outbreak, but I also think we’ll be able to contain it. I do not think that it’s possible to predict whether we’ll have a sustained outbreak. How long it will last and how broad it will be, we don’t know.
What were the most valuable lessons learned from dealing with the Ebola outbreak? Has that helped in dealing with the Zika epidemic?
They’re really too different. If there was a lesson, it was the importance of having a coordinated response and good communications between different elements of the response. We were not that successful with Ebola. The World Health Organization failed rather terribly with the Ebola outbreak. They admitted it. But we’re not seeing that with Zika. There seems to be much better coordination among health organizations with this disease.
What do you think is the greatest challenge that still exists in dealing with HIV and AIDS?
The challenge is the implementation of the advances we’ve already made. We now have excellent treatments and excellent capabilities at preventing infection. So we really have more of an implementation gap than we have a science gap. Certain parts of the country and the world are implementing programs very well, and we’re seeing a dramatic decrease in infection and death. In the United States, for example, there is a very robust program in San Francisco to aggressively seek out people, test them, get them into care, and keep them in care so that they save their own lives and don’t infect others. There are certain countries that are doing better than others. Rwanda, in Africa, is doing much better than other countries there. The implementation gap is really the big challenge.
But there are still some scientific challenges. We are trying very hard to get a good vaccine. We don’t have it yet. If and when we do get a good vaccine, it could play a major role in turning around the trajectory of the epidemic.
Given that, do you think there will be a day when we’ll be able to eliminate those diseases?
I think we’ll be able to control them much better than we can now. I think it’s too much to ask for to think that we can completely eradicate HIV. But we’d like to have control of HIV like we now do with many other infectious diseases.
What lessons have you learned from the recent epidemics that we’ve seen?
It’s the same lesson over and over again. You’ve got to be prepared. You have to have good surveillance. You have to have good diagnostics. And you have to be able to move quickly. And we’ve shown that when you do that, you get good results.
That’s the lesson.
Smithsonian magazine's "Future is Here" festival will be held April 22-24, 2016, at Shakespeare Theatre's Sidney Harman Hall in Washington, D.C. Exhilarating and visionary, the event will provide an eye-opening look into the near and far future, where science meets science fiction.
/https://tf-cmsv2-smithsonianmag-media.s3.amazonaws.com/accounts/headshot/randy-rieland-240.png)
/https://tf-cmsv2-smithsonianmag-media.s3.amazonaws.com/accounts/headshot/randy-rieland-240.png)