Video: Researchers Produce Human Tissue-Like Material Using 3D Printing
Using droplets coated in oil as “ink,” a 3D printer can construct a network of synthetic cells that mimics brain and fat tissue
![]()
What can’t a 3D printer build? The number of possible answers to this question has shrunk exponentially in recent years, as the high-tech machines continue to churn out solid object after object from computer designs.
The last few months alone saw countless new products and prototypes spanning an array of industries, from football cleats and pens to steel rocket parts and guns. Last month, the technology helped replace 75 percent of a person’s damaged skull, and this week it restored a man’s face after he lost half of it to cancer four years ago.
Today, a new study suggests 3D-printed material could one day mimic the behavior of cells in human tissue. Graduate student Gabriel Villar and his colleagues at the University of Oxford developed tiny solids that behave as biological tissue would. The delicate material physically resembles brain and fat tissue, and has the consistency of soft rubber.
To create this material, a specially designed 3D printing machine followed a computer programmed diagram and ejected tens of thousands of individual droplets according to a specified three-dimensional network. As seen in the video above, its nozzles moved in various angles to establish the position of each tiny bead. Each droplet weighs in at about one picoliter—that’s one trillionth of a liter—a unit used to measure the size of droplets of inkjet printers, whose nozzle technology works much the same way to consolidate tiny dots of liquid into complete images and words on paper.
The droplets of liquid contained biochemicals found in tissue cells. Coated in lipids—fats and oils—the tiny aqueous compartments stuck together, forming a cohesive and self-supporting shape, with each bead partitioned by a thin, single membrane similar to the lipid bilayers that protect our cells.
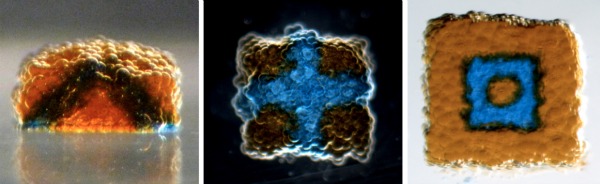
Several 3D-printed droplet networks. Image courtesy of Gabriel Villar, Alexander D. Graham and Hagan Bayley (University of Oxford)
The shapes that the printed droplets formed remained stable for several weeks. If researchers shook the material slightly, droplets could become displaced, but only temporarily. The engineered tissue quickly sprung back into its original shape, a level of elasticity the researchers say is comparable to soft tissue cells in humans. The intricate latticework of a network’s lipid bilayers appeared to hold the “cells” together.
In some of the droplet networks, the 3D printer built pores into the lipid membrane. The holes mimicked protein channels inside the barriers that protect real cells, filtering molecules important for cell function in and out. The researchers injected into the pores a type of molecule important for cell-to-cell communication, one that delivers signals to numerous cells so that they function together as a group. While the 3D-printed material couldn’t exactly replicate how cells propagate signals, researchers say the movement of the molecule through defined pathways resembled the electrical communication of neurons in brain tissue
Water readily permeated the network’s membranes, even when pores were not built into its structure. The droplets swelled and shrank by the process of osmosis, trying to establish equilibrium between the amount of water they contained and the amount surrounding them on the outside. The movement of water was enough to lift the droplets against gravity, pulling and folding them, imitating muscle-like activity in human tissue.
The researchers hope that these droplet networks could be programmed to release drugs following a physiological signal. Printed cells could someday also be integrated into damaged or failing tissue, providing extra scaffolding or even replacing malfunctioning cells, perhaps even supplanting some of the 1.5 million tissue transplants that take place in the United States each year. The potential seems greatest for brain tissue transplants, as medical engineers are currently trying to grow brain cells in the lab to treat progressive diseases like Huntington’s disease, which slowly destroys nerve cells.
Whether it’s growing human tissue or entire ears, 3D printing technology is in full swing in the field of medicine, and countless researchers will no doubt jump on the bandwagon in the coming years.
/https://tf-cmsv2-smithsonianmag-media.s3.amazonaws.com/accounts/headshot/marina-koren-240.jpg)
/https://tf-cmsv2-smithsonianmag-media.s3.amazonaws.com/accounts/headshot/marina-koren-240.jpg)