How Our Brains Make Memories
Surprising new research about the act of remembering may help people with post-traumatic stress disorder
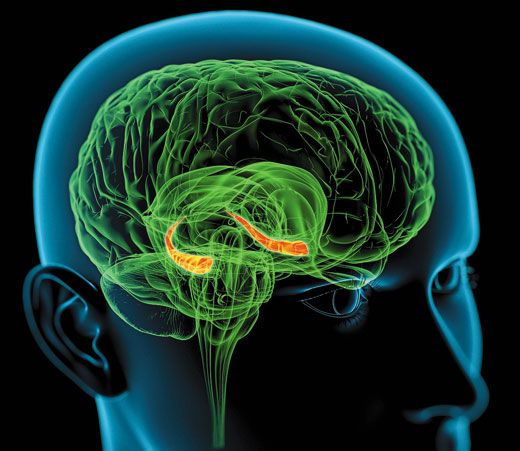
/https://tf-cmsv2-smithsonianmag-media.s3.amazonaws.com/filer/Memory-hippocampus-brain-631.jpg)
Sitting at a sidewalk café in Montreal on a sunny morning, Karim Nader recalls the day eight years earlier when two planes slammed into the twin towers of the World Trade Center. He lights a cigarette and waves his hands in the air to sketch the scene.
At the time of the attack, Nader was a postdoctoral researcher at New York University. He flipped the radio on while getting ready to go to work and heard the banter of the morning disc jockeys turn panicky as they related the events unfolding in Lower Manhattan. Nader ran to the roof of his apartment building, where he had a view of the towers less than two miles away. He stood there, stunned, as they burned and fell, thinking to himself, “No way, man. This is the wrong movie.”
In the following days, Nader recalls, he passed through subway stations where walls were covered with notes and photographs left by people searching desperately for missing loved ones. “It was like walking upstream in a river of sorrow,” he says.
Like millions of people, Nader has vivid and emotional memories of the September 11, 2001, attacks and their aftermath. But as an expert on memory, and, in particular, on the malleability of memory, he knows better than to fully trust his recollections.
Most people have so-called flashbulb memories of where they were and what they were doing when something momentous happened: the assassination of President John F. Kennedy, say, or the explosion of the space shuttle Challenger. (Unfortunately, staggeringly terrible news seems to come out of the blue more often than staggeringly good news.) But as clear and detailed as these memories feel, psychologists find they are surprisingly inaccurate.
Nader, now a neuroscientist at McGill University in Montreal, says his memory of the World Trade Center attack has played a few tricks on him. He recalled seeing television footage on September 11 of the first plane hitting the north tower of the World Trade Center. But he was surprised to learn that such footage aired for the first time the following day. Apparently he wasn’t alone: a 2003 study of 569 college students found that 73 percent shared this misperception.
Nader believes he may have an explanation for such quirks of memory. His ideas are unconventional within neuroscience, and they have caused researchers to reconsider some of their most basic assumptions about how memory works. In short, Nader believes that the very act of remembering can change our memories.
Much of his research is on rats, but he says the same basic principles apply to human memory as well. In fact, he says, it may be impossible for humans or any other animal to bring a memory to mind without altering it in some way. Nader thinks it’s likely that some types of memory, such as a flashbulb memory, are more susceptible to change than others. Memories surrounding a major event like September 11 might be especially susceptible, he says, because we tend to replay them over and over in our minds and in conversation with others—with each repetition having the potential to alter them.
For those of us who cherish our memories and like to think they are an accurate record of our history, the idea that memory is fundamentally malleable is more than a little disturbing. Not all researchers believe Nader has proved that the process of remembering itself can alter memories. But if he is right, it may not be an entirely bad thing. It might even be possible to put the phenomenon to good use to reduce the suffering of people with post-traumatic stress disorder, who are plagued by recurring memories of events they wish they could put behind them.
Nader was born in Cairo, Egypt. His Coptic Christian family faced persecution at the hands of Arab nationalists and fled to Canada in 1970, when he was 4 years old. Many relatives also made the trip, so many that Nader’s girlfriend teases him about the “soundtrack of a thousand kisses” at large family gatherings as people bestow customary greetings.
He attended college and graduate school at the University of Toronto, and in 1996 joined the New York University lab of Joseph LeDoux, a distinguished neuroscientist who studies how emotions influence memory. “One of the things that really seduced me about science is that it’s a system you can use to test your own ideas about how things work,” Nader says. Even the most cherished ideas in a given field are open to question.
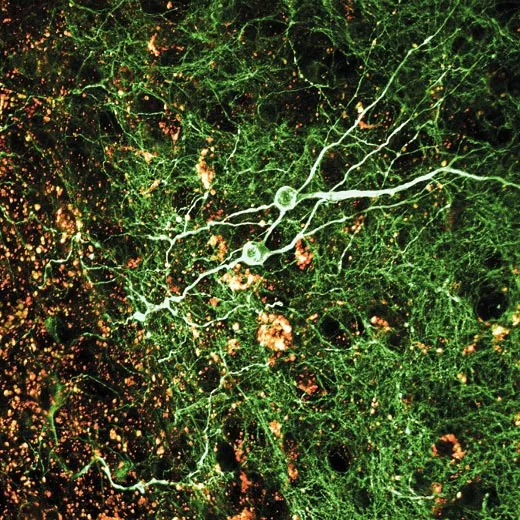
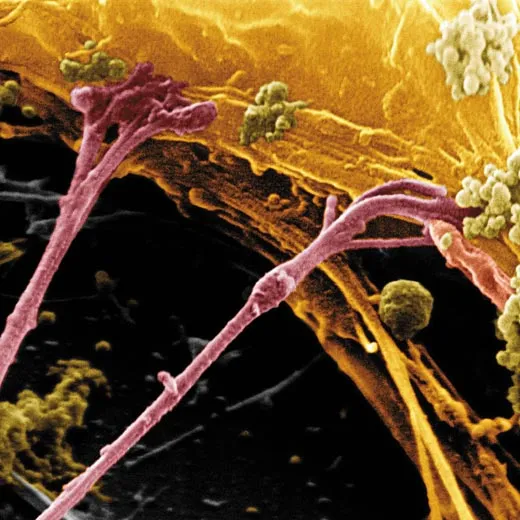
Scientists have long known that recording a memory requires adjusting the connections between neurons. Each memory tweaks some tiny subset of the neurons in the brain (the human brain has 100 billion neurons in all), changing the way they communicate. Neurons send messages to one another across narrow gaps called synapses. A synapse is like a bustling port, complete with machinery for sending and receiving cargo—neurotransmitters, specialized chemicals that convey signals between neurons. All of the shipping machinery is built from proteins, the basic building blocks of cells.
One of the scientists who has done the most to illuminate the way memory works on the microscopic scale is Eric Kandel, a neuroscientist at Columbia University in New York City. In five decades of research, Kandel has shown how short-term memories—those lasting a few minutes—involve relatively quick and simple chemical changes to the synapse that make it work more efficiently. Kandel, who won a share of the 2000 Nobel Prize in Physiology or Medicine, found that to build a memory that lasts hours, days or years, neurons must manufacture new proteins and expand the docks, as it were, to make the neurotransmitter traffic run more efficiently. Long-term memories must literally be built into the brain’s synapses. Kandel and other neuroscientists have generally assumed that once a memory is constructed, it is stable and can’t easily be undone. Or, as they put it, the memory is “consolidated.”
According to this view, the brain’s memory system works something like a pen and notebook. For a brief time before the ink dries, it’s possible to smudge what’s written. But after the memory is consolidated, it changes very little. Sure, memories may fade over the years like an old letter (or even go up in flames if Alzheimer’s disease strikes), but under ordinary circumstances the content of the memory stays the same, no matter how many times it’s taken out and read. Nader would challenge this idea.
In what turned out to be a defining moment in his early career, Nader attended a lecture that Kandel gave at New York University about how memories are recorded. Nader got to wondering about what happens when a memory is recalled. Work with rodents dating back to the 1960s didn’t jibe with the consolidation theory. Researchers had found that a memory could be weakened if they gave an animal an electric shock or a drug that interferes with a particular neurotransmitter just after they prompted the animal to recall the memory. This suggested that memories were vulnerable to disruption even after they had been consolidated.
To think of it another way, the work suggested that filing an old memory away for long-term storage after it had been recalled was surprisingly similar to creating it the first time. Both building a new memory and tucking away an old one presumably involved building proteins at the synapse. The researchers had named that process “reconsolidation.” But others, including some prominent memory experts, had trouble replicating those findings in their own laboratories, so the idea wasn’t pursued.
Nader decided to revisit the concept with an experiment. In the winter of 1999, he taught four rats that a high-pitched beep preceded a mild electric shock. That was easy—rodents learn such pairings after being exposed to them just once. Afterward, the rat freezes in place when it hears the tone. Nader then waited 24 hours, played the tone to reactivate the memory and injected into the rat’s brain a drug that prevents neurons from making new proteins.
If memories are consolidated just once, when they are first created, he reasoned, the drug would have no effect on the rat’s memory of the tone or on the way it would respond to the tone in the future. But if memories have to be at least partially rebuilt every time they are recalled—down to the synthesizing of fresh neuronal proteins—rats given the drug might later respond as if they had never learned to fear the tone and would ignore it. If so, the study would contradict the standard conception of memory. It was, he admits, a long shot.
“Don’t waste your time, this will never work,” LeDoux told him.
It worked.
When Nader later tested the rats, they didn’t freeze after hearing the tone: it was as if they’d forgotten all about it. Nader, who looks slightly devilish in his earring and pointed sideburns, still gets giddy talking about the experiment. Eyes wide with excitement, he slaps the café table. “This is crazy, right? I went into Joe’s office and said, ‘I know it’s just four animals, but this is very encouraging!’”
After Nader’s initial findings, some neuroscientists pooh-poohed his work in journal articles and gave him the cold shoulder at scientific meetings. But the data struck a more harmonious chord with some psychologists. After all, their experiments had long suggested that memory can easily be distorted without people realizing it.
In a classic 1978 study led by Elizabeth Loftus, a psychologist then at the University of Washington, researchers showed college students a series of color photographs depicting an accident in which a red Datsun car knocks down a pedestrian in a crosswalk. The students answered various questions, some of which were intentionally misleading. For instance, even though the photographs had shown the Datsun at a stop sign, the researchers asked some of the students, “Did another car pass the red Datsun while it was stopped at the yield sign?”
Later the researchers asked all the students what they had seen—a stop sign or yield sign? Students who’d been asked a misleading question were more likely to give an incorrect answer than the other students.
To Nader and his colleagues, the experiment supports the idea that a memory is re-formed in the process of calling it up. “From our perspective, this looks a lot like memory reconsolidation,” says Oliver Hardt, a postdoctoral researcher in Nader’s lab.
Hardt and Nader say something similar might happen with flashbulb memories. People tend to have accurate memories for the basic facts of a momentous event—for example, that a total of four planes were hijacked in the September 11 attacks—but often misremember personal details such as where they were and what they were doing at the time. Hardt says this could be because these are two different types of memories that get reactivated in different situations. Television and other media coverage reinforce the central facts. But recalling the experience to other people may allow distortions to creep in. “When you retell it, the memory becomes plastic, and whatever is present around you in the environment can interfere with the original content of the memory,” Hardt says. In the days following September 11, for example, people likely repeatedly rehashed their own personal stories—“where were you when you heard the news?”—in conversations with friends and family, perhaps allowing details of other people’s stories to mix with their own.
Since Nader’s original experiment, dozens of studies with rats, worms, chicks, honeybees and college students have suggested that even long-standing memories can be disrupted when recalled. Nader’s goal is to tie the animal research, and the clues it yields about the bustling molecular machinery of the synapse, to the everyday human experience of remembering.
Some experts think he is getting ahead of himself, especially when he makes connections between human memory and these findings in rats and other animals. “He oversells it a little bit,” says Kandel.
Daniel Schacter, a psychologist at Harvard University who studies memory, agrees with Nader that distortions can occur when people reactivate memories. The question is whether reconsolidation—which he thinks Nader has demonstrated compellingly in rat experiments—is the reason for the distortions. “The direct evidence isn’t there yet to show that the two things are related,” Schacter says. “It’s an intriguing possibility that people will now have to follow up on.”
A real-world test of Nader’s theory of memory reconsolidation is taking place a few miles from his Montreal office, at the Douglas Mental Health University Institute. Alain Brunet, a psychologist, is running a clinical trial involving people with post-traumatic stress disorder (PTSD). The hope is that caregivers might be able to weaken the hold of traumatic memories that haunt patients during the day and invade their dreams at night.
Brunet knows how powerful traumatic memories can be. In 1989, when he was studying for a master’s degree in psychology at the University of Montreal, a man armed with a semiautomatic rifle walked into an engineering classroom on campus, separated the men from the women and shot the women. The gunman continued the massacre in other classrooms and hallways of the university’s École Polytechnique, shooting 27 people and killing 14 women before killing himself. It was Canada’s worst mass shooting.
Brunet, who was on the other side of campus that day, says, “this was a very powerful experience for me.” He says he was surprised to discover how little was known at the time about the psychological impact of such events and how to help people who’ve lived through them. He decided to study traumatic stress and how to treat it.
Even now, Brunet says, the drugs and psychotherapy conventionally used to treat PTSD do not provide lasting relief for many patients. “There’s still plenty of room for the discovery of better treatments,” he says.
In Brunet’s first study, PTSD patients took a drug intended to interfere with the reconsolidation of fearful memories. The drug, propranolol, has long been used to treat high blood pressure, and some performers take it to combat stage fright. The drug inhibits a neurotransmitter called norepinephrine. One possible side effect of the drug is memory loss. (In a study similar to Nader’s original experiment with rats, researchers in LeDoux’s lab have found that the drug can weaken fearful memories of a high-pitched tone.)
The patients in Brunet’s study, published in 2008, had each experienced a traumatic event, such as a car accident, assault or sexual abuse, about a decade earlier. They began a therapy session sitting alone in a nondescript room with a well-worn armchair and a television. Nine patients took a propranolol pill and read or watched TV for an hour as the drug took effect. Ten were given a placebo pill.
Brunet came into the room and made small talk before telling the patient he had a request: he wanted the patient to read a script, based on earlier interviews with the person, describing his or her traumatic experience. The patients, all volunteers, knew that the reading would be part of the experiment. “Some are fine, some start to cry, some need to take a break,” Brunet says.
A week later, the PTSD patients listened to the script, this time without taking the drug or a placebo. Compared with the patients who had taken a placebo, those who had taken the propranolol a week earlier were now calmer; they had a smaller uptick in their heart rate and they perspired less.
Brunet has just completed a larger study with nearly 70 PTSD patients. Those who took propranolol once a week for six weeks while reading the script of their traumatic event showed an average 50 percent reduction in standard PTSD symptoms. They had fewer nightmares and flashbacks in their daily lives long after the effects of the drug had worn off. The treatment didn’t erase the patients’ memory of what had happened to them; rather, it seems to have changed the quality of that memory. “Week after week the emotional tone of the memory seems weaker,” Brunet says. “They start to care less about that memory.”
Nader says the traumatic memories of PTSD patients may be stored in the brain in much the same way that a memory of a shock-predicting tone is stored in a rat’s brain. In both cases, recalling the memory opens it to manipulation. Nader says he’s encouraged by the work so far with PTSD patients. “If it’s got any chance of helping people, we have to give it a shot,” he says.
Among the many questions that Nader is now pursuing is whether all memories become vulnerable when recalled, or only certain memories under certain circumstances.
Of course, there is the even bigger question: why are memories so unreliable? After all, if they were less subject to change we wouldn’t suffer the embarrassment of misremembering the details of an important conversation or a first date.
Then again, editing might be another way to learn from experience. If fond memories of an early love weren’t tempered by the knowledge of a disastrous breakup, or if recollections of difficult times weren’t offset by knowledge that things worked out in the end, we might not reap the benefits of these hard-earned life lessons. Perhaps it’s better if we can rewrite our memories every time we recall them. Nader suggests that reconsolidation may be the brain’s mechanism for recasting old memories in the light of everything that has happened since. In other words, it just might be what keeps us from living in the past.
Greg Miller writes about biology, behavior and neuroscience for Science magazine. He lives in San Francisco. Gilles Mingasson is a photographer based in Los Angeles.