Space Station ER
What happens if an astronaut in space needs surgery?
:focal(2107x871:2108x872)/https://tf-cmsv2-smithsonianmag-media.s3.amazonaws.com/filer/6c/d6/6cd696ff-d57b-4d2c-921b-e27861e09cf1/06d_sep2015_hermeticsurgerya_live.jpg)
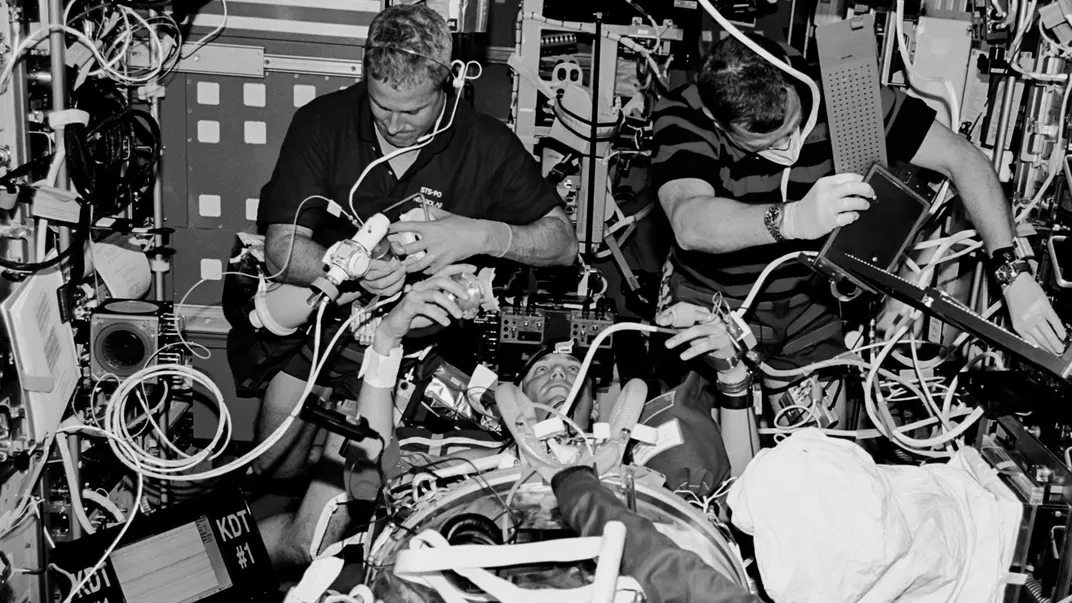
Aboard an ancient Boeing KC-135 nicknamed the “Vomit Comet,” a medical research team goes to work as the NASA aircraft flies a parabolic curve, entering a 25-second period of zero gravity. To avoid floating away, surgeon Mark R. Campbell wedges his feet beneath a bar at the base of a prototype surgical table. Atop the table lies an anesthetized and rigidly restrained rabbit, Campbell’s research subject. This test is the culmination of six months of planning.
Campbell ignores the sensation of weightlessness as he takes a scalpel and carefully opens the rabbit’s carotid artery, then pulls back to watch. Initially, Campbell sees exactly what he expects. In zero gravity, bright red globes of blood streak out of the wound like paint balls fired from a gun. But within seconds, the steady flow of globes diminishes and then stops while a dome of blood grows over the incision. Dismayed, Campbell makes his carotid incision larger to increase blood flow but the results are unchanged, and a cut into a major artery in the rabbit’s abdomen has the same result. “Finally we just figured out that that’s the way blood acts in weightlessness,” he says. “It didn’t act the way we thought it would.”
In five decades of human spaceflight and 15 years of continuous occupation of the International Space Station, no human has ever undergone a surgical procedure in orbit. Given the intent of national space agencies, private companies, and even some individuals to launch long-range space missions, it seems inevitable that at some point someone will have a bad day, and surgery will be needed to save a life. When that day comes, the patient may want to send Campbell a thank-you note.
Campbell’s 1991 rabbit experiment took place during the buildup for Space Station Freedom, which was to have been a gigantic outpost, with a 1,200-pound, X-ray–equipped module that could address almost any medical emergency. The well-stocked space ER was a necessity because of the space shuttle’s expected launch schedule—once every 45 days. Though a patient on the ground could be brought to a hospital within minutes, in space it was conceivable that for 45 days, an incapacitated or badly hurt astronaut would have to suffer without support from Earthbound doctors and equipment. “That was a really long time,” says Campbell.
A retired NASA flight surgeon, Campbell is a member of the FAA’s Commercial Space Transportation Advisory Committee and a practicing general surgeon in Paris, Texas. Because no one was sure if surgery in zero gravity was possible, his experiment on bleeding behavior was an early step in a new world. By the time the parabolic flights concluded, in 2000, Campbell had attempted procedures ranging from simple sutures and CPR to laparoscopy while floating in brief periods of zero gravity. By that time NASA faced the reality of far fewer shuttle launches with much more time between, and Freedom morphed into the smaller International Space Station, and most of the planned medical capabilities were shelved.
Aboard the International Space Station, the care available to the permanent crew of six is minimal. There are ventilation devices to assist breathing, a defibrillator for heart problems, a folding patient restraint table that doubles as a transport device. An ultrasound-imaging device, meant for scientific research, could in a pinch be used for diagnostics. The medical kit can handle relatively minor ailments but simply cannot cope with disaster. No matter the equipment, the crew may be unable to handle the situation. Even qualified doctors that fly may be too out of practice to perform.
“They are trained to treat someone who is choking; we have a procedure where they respond to toxic exposure; we can treat a seizure, chest pain…. Most of these things do not require any surgical-type intervention—it’s a simple procedure like putting in an airway,” says Terry Taddeo, NASA’s current chief of space medicine. “If they reported something they didn’t feel comfortable with, we would get the people in [mission control] that could assist, talk them through it.” Rather than a sophisticated medical suite, the ISS keeps a spare Russian Soyuz capsule for use as a lifeboat, with the treatment plan being a ride home within 24 hours. Strapped into the Soyuz’s confines, astronauts experience up to 8 Gs during a reentry, which makes it one of the roughest ambulance rides anyone is likely to experience.
In the economics of space research, the cold fact is that any medical capability launched comes at the expense of something else, so agencies launch only as much as they feel they can get away with. Prospective astronauts are subjected to an intense selection process, and those at risk for even minor medical conditions are weeded out, minimizing the chances that weighty medical equipment is needed.
“If we’re going to orbit, that’s like going on a camping trip,” says Linda Plush, a nurse practitioner and co-founder of the Space Nursing Society. “So I’m not going to take the kitchen sink. I’m going to look at what’s common, what’s likely to occur, and prepare for that.”
But a deep-space mission, like to Mars or beyond, changes the calculations. An exploration spacecraft will end up so far away that evacuation will be all but impossible. “If you have surgical capabilities, the question is where do you draw the line?” asks astronaut Mike Barratt, a physician who has been on two ISS missions. “Are you going to always have a doctor on board? That means that one-sixth of the astronaut office has to be a clinically current surgeon.”
Because the astronauts have no discernible medical problems, Barratt believes the most likely reason for surgery will be a wound. “When you think about what brings people to the ER on the ground, it’s traumatic forces. It’s falls, it’s motor vehicle accidents, it’s gunshot wounds and industrial accidents. [In space] we don’t have motor vehicles. We don’t have falls because there’s no gravity. We don’t have gunshots. So then you’re down to industrial accident-type things and shrapnel.”
But would you even want to perform a medical procedure aboard the ISS? “If you sneeze, if you go to the bathroom and you have bad technique, or if eating and you’re a messy eater—all that stuff goes into the atmosphere for your compadres to breathe,” explains ISS veteran Barratt. “And everybody sheds dead skin at a high rate in space, and that one’s of the things we see a lot in the fan filters and the filter intakes…. So we aren’t anywhere near as clean as an operating room.”
“If you do an operation,” says surgeon Mark Campbell, “wouldn’t that mean your risk of infection would be higher because you’ve got all these nasty particles floating around? Well, no one knows.”
Tinier particles are a risk too. In the closed environment of a spacecraft, exhaled molecules of anesthetic would become a permanent part of the air the crew breathes, so there is no way they wouldn’t inhale molecules of anesthetic gas. When an anesthetic is needed, the inhabitants are limited to drugs that can be injected or swallowed.
Not that we understand quite how medicines work in space. On Earth some medications are sensitive to light or temperature; with extra radiation and changes to the human body, much remains unknown. For that matter, some germs and bacteria don’t act like they do on Earth. In low Earth orbit some organisms seem less virulent and others more so, and we don’t really understand why. Even less is known about their behaviors in the radiation-filled environment of deep space. “The drugs we use in space, we use at dosages we use on Earth,” says Campbell. “And basically we say, ‘We don’t know what the [space] effects are so we’re not gonna take them into account.’ ”
“So then the question becomes: Is the dose needed to control [an] infection a lethal dose, [or] will it even work?” asks nurse-practioner Linda Plush, who has consulted with NASA on drug issues. “I can’t honestly tell you too much about medications in space, other than I know cosmic radiation causes some problems and we’re just not sure. There haven’t been enough studies done to even begin to answer that question.”
One way to minimize infections is to limit exposure through laparoscopy, a surgical technique that uses small incisions and miniaturized tools to work inside the body. In laparoscopy, the body serves as its own surgical enclosure, keeping germs and debris out while keeping blood and other body fluids in. It’s one of the techniques that Campbell tested aboard the Vomit Comet, successfully performing abdominal surgery on a 100-pound pig. But the equipment is bulky and power-hungry, and if problems develop, the surgeon must be able to carry on in traditional, open surgical techniques. The procedure is also difficult. “I think that all you need [for conventional surgery] is a little bit of training and a little bit of minimal equipment and you can do a lot, and do it very effectively,” says Campbell. “If you do laparoscopy, not only do you have to have a lot of equipment, you have to have a lot of training. We’re talking about years and years of training.”
In 2014, a medical device company announced a tiny new robotic device that could be placed inside the human body to perform surgery; it was billed as having great potential for spaceflight. Campbell, who performs hundreds of robotic surgeries a year, is not buying it: “I can promise you that an appendectomy is 10 times harder robotically than open, takes 20 times the equipment, and 40 times the training.”
Even if astronauts have the most advanced robotics for surgery, there will be crises when it will be useless. “Let’s say a piece of orbital debris punctured a spacesuit, penetrated, and hit a major [blood] vessel. Then that’s something that there’s no way we would be able to treat...so we make no provision for it whatsoever,” says Campbell. “And the list goes on and on. There are fairly obvious things that would exceed the medical care system and we would just say ‘We can’t take care of that. If that happens, you’re gonna die.’ These are things that are mostly of low incidence, but really bad, serious outcomes.”
“We look our program managers in the eye and we come up with our best discretionary line on medical capability. And on the other side of that line, someone is gonna die,” acknowledges Barratt.
No doubt one of the toughest decisions will be faced when an astronaut cannot be saved but may linger for some time before dying. An astronaut who is suffering could consume a spacecraft’s entire supply of a vital medicine before expiring, which could threaten crewmates who would otherwise survive their own medical issues. Would the commander then have to choose between treating the fatally injured astronaut and protecting the rest of the crew? Then the question becomes: What to do with a body?
“There’s been a lot of discussion on that,” Campbell answers. “You’d probably ‘bury’ them in space. You’d probably put them in the airlock and put them out into space.” An official procedure exists, but exactly what would happen depends on consultations between the crew, the family and mission control.
Everyone agrees that a mission to Mars and beyond will be dangerous, and to Barratt the biggest unsolved medical hurdle is deep-space radiation, a problem NASA hopes to solve with an as-yet-undeveloped shielding. But to Campbell, the biggest hurdle something that no surgeon or high-tech device can fix: How will six people handle living in something not much bigger than a bus for as long as three years?