Killer at 70,000 Feet
The occupational hazards of flying the U-2
:focal(312x114:313x115)/https://tf-cmsv2-smithsonianmag-media.s3.amazonaws.com/filer/e5/e4/e5e4e93a-5f2d-4dcf-b9bd-6f2306de23a0/killer_at_70000_feet_2_flashjpg__800x600_q85_crop.jpg)
United States Air Force Lieutenant Colonel Kevin Henry thought the tiny red dots on his skin were insect bites. But as he relaxed at a Florida beach house with a fellow pilot on a day off in 1990, he noticed he was the only one getting bitten. Henry wouldn’t learn until later that the dots were capillaries breaking under the strain of nitrogen bubbles that had formed during his latest flight in a Lockheed U-2 spyplane, 10 hours earlier. He would find out the hard way how much worse it could get.
Henry had been flying the U-2 since 1987, and has seen it go from flying over South Korea and Panama to being a constant presence over battlefields in Afghanistan and, until last year, Iraq. Like most others in the elite club of U-2 pilots (there are only 35 to 50 actively flying at any time), Henry is tough and matter-of-fact, but also somewhat romantic about flying the famous jet at 70,000 feet, twice the cruising altitude of commercial airliners—high enough to see the curvature of Earth.
But flying so high has a cost. The dots that Henry saw on his skin and the itching, crawling sensation that he felt were just a couple of the symptoms of altitude-induced decompression sickness. Most people know DCS by its common name, the bends, a condition suffered by divers who rise too quickly from the high pressure at depth to the lower pressure near the water’s surface. (In medical terms, “bends” refers only to the DCS sufferer’s joint pain.)
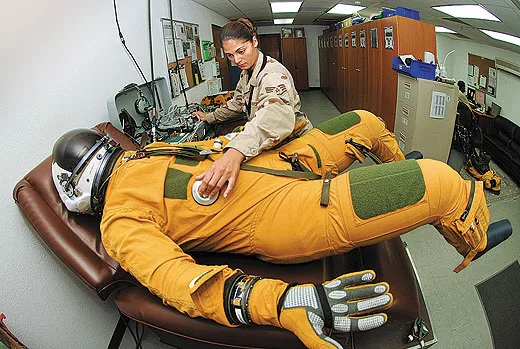
Pilots can experience the same physical reactions by flying up into the thin air at high altitudes. U-2 pilots are especially at risk, not just because of their extreme altitude but also because their cockpits are only partially pressurized. The pressure in a U-2 cockpit at typical mission altitude is equivalent to the atmosphere at 29,000 feet—as high as the summit of Mt. Everest. To cope, U-2 pilots breathe pure oxygen for an hour before their flight and wear a kind of pressurized spacesuit. Pre-breathing oxygen helps purge nitrogen from their bodies. If nitrogen remains even after pre-breathing and the pilot goes up, the thin atmosphere will cause the nitrogen dissolved in the body’s blood and tissue to essentially boil. The same principle is at work when you open a can of soda: Release the pressure and the dissolved gas rushes to escape, in the form of bubbles. In the human body, bubbles can cause extreme pain, bruising, brain damage, and, without treatment, death.
In March 2006, Henry started experiencing symptoms more severe than the itchy dots he’d had 16 years earlier. This time, however, he was several hours into a combat mission, in support of Operation Enduring Freedom in the Middle East, and more than 13 miles above the ground. “The first thing that happened was the pain in my knees,” he says. “I kind of blew it off because it was very, very light. But this was bilateral”—the pain was in both knees. “They never taught us before: Bilateral is bad. So I just pressed on, of course; that’s what we do.”
Over the next five hours, Henry developed an intense headache, nausea, and extreme fatigue. The pain got worse. At one point, he hallucinated that the airplane had rolled 30 degrees to the left. He began to feel disoriented and sluggish, a sensation he likens to intoxication. At one point, he snapped awake, not realizing he’d dozed off.
“That’s when I go, Okay, I’m not feeling well, and I had to fess up,” he says. He hadn’t wanted to be grounded due to what he thought was an inconsequential medical problem, or to let the younger pilots hear that he returned complaining of a mere headache.
Henry contacted his ground mission supervisor, who woke up the squadron commander back at Beale Air Force Base in California. By that point, Henry had essentially forgotten how to fly his airplane.
Like Henry’s red dots, many symptoms of DCS don’t show up until after a pilot has landed, sometimes days later. The symptoms can be as minor as a headache or fatigue, so they’re often ignored or attributed to dehydration, lack of sleep, even caffeine withdrawal. Says Henry: “We didn’t talk about it, because back when I was growing up in the program it was like ‘Oh, you’ll get grounded.’ ”
Even though pilots were cautious never to appear too sick to fly, true DCS cases also used to be somewhat rare, and severe cases almost unheard of. Pre-breathing oxygen and a strict regimen of rest between flights were enough to keep pilots healthy. For decades, it was enemy fire, not nitrogen bubbles, that worried them.
But the U-2 program has seen more cases of DCS over the last decade than at any other time in its 56-year history. Since the war in Afghanistan started, in 2001, the average number of cases reported each year has almost doubled. More important, before 2002, no cases severe enough to hinder U-2 operations were reported, but between 2002 and 2009, there were 16 confirmed severe cases, five of which were deemed life-threatening. Nine of the pilots who experienced serious DCS symptoms reported long-lasting or permanent brain damage.
A study published in the July 2011 issue of the journal Aviation, Space, and Environmental Medicine analyzed 40 years of the military’s medical records to find possible reasons for the shift. Three major factors seem to be contributing to the increase. First, pilots are flying more often. With a demanding new role—providing ground combat support in Afghanistan—U-2 pilots are flying 70 percent more hours on 122 percent more sorties than they did during the cold war.
U-2 pilots are also flying for longer stretches. During the cold war, flights rarely lasted longer than eight hours; now ground operations require U-2s to stay in the air for up to 12 hours. As a result, severe DCS cases over the last decade are concentrated among the pilots flying out of the primary support base for combat operations in Iraq and Afghanistan.
Finally, fundamental changes in the work pilots are doing may also be making things worse. The study found that even mild exercise, including motions as simple as pressing foot pedals or raising an arm to flip a switch, can greatly increase the risk of DCS. Unlike cold war reconnaissance, today’s missions require pilots to do much more in the cockpit—operating a radio, inputting navigational data, adjusting sensors—so the new mission itself could be partly responsible for releasing nitrogen bubbles through a pilot’s bloodstream.
Lieutenant Colonel Sean Jersey, a physician and one of the study’s authors, cites a potential fourth factor: stress. In the Soviet flyover days, U-2 pilots would head out to a target, snap pictures, and fly back. They could even sleep part of the way, letting the airplane fly on autopilot. Today, pilots must quickly react to changes on the battlefield, acting as a mobile relay station for communications and an eye in the sky for troops fighting on difficult terrain. They’re also in constant contact with the soldiers on the ground, often during combat.
“Emotionally, I think they’re wrung out from that,” says Jersey. “When you’re talking to somebody on the radio and there’s gunfire in the background…you’re not taking a nap while that’s happening.”
Lieutenant Colonel Blake Smith is a U-2 pilot who retired early last year. He often served as director of operations for the 99th Expeditionary Reconnaissance Squadron, to which the U-2 is assigned, during the shift toward combat support missions, and he knew the pilots and their problems well. He remembers that when he joined the program in 1998, DCS was mostly a non-issue. Pilots might complain of minor joint pain, but once they were back on the ground and rested, their symptoms would generally get better.
“Years ago, whenever you mentioned you had a little bit of DCS, the reaction from the medical forces, and the reaction from the Air Force for that matter, was not as thorough and robust as it is now,” says Smith.
What changed, he says, was the sudden appearance of DCS cases that affected the pilots’ central nervous systems, something no one in the program was used to handling. On the way home from flying a long-duration combat mission for Enduring Freedom in late 2002, Major Greg Kimbrough suffered severe symptoms. Having been trained to expect joint pain and a headache, he had no idea that his inability to read fine print or recognize his landing field was indicative of decompression sickness. “What we got when we went through our initial training was the basics of it,” says Kimbrough, “and that was all based on past events,” when the cases were minor.
By the time he was having major symptoms at altitude, Kimbrough’s cognition was so compromised that it never occurred to him to call for help. Somehow he was able to land his U-2 safely, but he has little memory of the last hours of the flight.
Kimbrough was one of the first U-2 pilots to experience central nervous system DCS, also called Type II DCS. In the following months more cases cropped up. The Air Force took notice, but because flight doctors still didn’t understand exactly how and why DCS affects pilots, they were slow to find ways of coping with the new threat. Air Force physiologists pored over Kimbrough’s equipment, trying to find out why the normal pre-breathe precautions had failed. Pilots were told to pre-breathe for a longer time, but they weren’t given more rest between flights. The wars in Iraq and Afghanistan continued, the missions stayed long, and pilots continued to get sick.
According to Jersey, the Air Force’s attitude toward DCS changed significantly in 2006. He thinks the squadron was overconfident in the attention they were paying DCS prevention, “until Kevin Henry really woke everybody up.”
Henry had already vomited into his pressure-sealed helmet by the time his squadron commander got on the data link, the U-2’s upgraded version of a radio. Henry had to take off the helmet so he could see, exposing his body to the much lower pressure in the cabin and further accelerating the development of symptoms. He tried putting coordinates for his home base into the autopilot, then realized he had forgotten how to use the device. Lieutenant Colonel Dave Russell, the squadron commander, had just gotten out of bed back in California, and began to talk Henry through the process of getting home.
Over the next three hours, with Russell’s guidance, Henry managed to steer his U-2 toward a friendly air base in the Middle East. His short-term memory was gone; all he had to rely on was the muscle memory he’d developed as a young trainee. “I could still do basic airmanship stuff,” he says, “you know, push forward on the yoke and the houses get bigger.”
But even simple tasks were getting harder. As Henry neared the runway, Russell told him to put the landing gear down. When he reached for the handle, it wasn’t there. He’d developed several blind spots in his vision, and had to grope around in the area where he knew the handle should be.
“Nothing made any sense,” he says. “I had horns and lights going off, and I go, That means something important—I can’t remember what that light means.”
Henry doesn’t remember the last 45 minutes of the flight. People watching from the ground later described to him the way he plummeted toward bunkers and hangars, sending ground crews running. When it became clear that Henry didn’t know what to do next, a pair of Mirage jet fighters from the local air force helped to guide him down toward the runway.
After a number of unsuccessful landing attempts, Henry blacked out again, this time while headed straight for the ground.
“It was almost like it faded in,” he says about the scene in front of him. “And there was a bunker in the middle of the windscreen. And just instinctively [I] did a traffic pattern stall recovery. You know, stuff that you learn from day one flying.” An adrenaline rush momentarily cleared his head, and he pulled the airplane around and landed it in the middle of the runway. When the U-2 came to a stop, pilots on the ground had to drag Henry’s limp body from the cockpit.
He wasn’t out of the woods yet. Nitrogen gas had already ravaged his body; the treatment for people suffering from DCS is usually administered much earlier in the process. He was placed in a hyperbaric chamber, a pressurized room where a gradual shift from low to high pressure gives nitrogen gas time to dissolve back into the blood. For several days, he was in and out of the chamber, still in a haze and unable to remember simple things, like how to fasten a seat belt. Despite having been close to death, Henry recovered fully from his physical symptoms. The only visible evidence of his ordeal are scars that the bubbling nitrogen left on his skin.
Despite the recommendation of the neurologist who assessed him after the 2006 incident, Henry was cleared to fly with no restrictions. Smith acknowledges that he, too, saw pilots who continued to suffer from the effects of their DCS episodes even after they were cleared. Kimbrough says he felt fine to fly, but was still a little surprised the Air Force sent him back up to high altitude only six months after his incident. “I only know they needed me,” he says.
A few months after he was cleared to fly, Henry had another brush with central nervous system DCS. At high altitude, he suddenly had the sensation of free-falling. Though completely awake, he slumped over in his seat, unable to move. He recovered and landed safely, but it quickly became clear that DCS had taken its toll on his brain. He was grounded permanently, and today has problems with short-term memory and reasoning.
In 2008, two years after Henry’s incidents, the increasing frequency and severity of DCS cases among U-2 pilots prompted Jersey and his colleagues to look through the Air Force’s medical records to see if they could find a pattern. As a new flight doctor at Beale, Jersey saw a DCS case his first week, and another soon after. He quickly realized that the Air Force had a serious problem. He and the other flight doctors, along with the squadron commander, went to Air Combat Command to request an investigation. A panel was formed to conduct a study and recommend what to do next.
Jersey points out that the study is based on military records alone, which are often inconsistent and can’t substitute for proper observation of the incidence of DCS. It is also possible that the increase in the DCS cases reported is partly due to a change in culture within the U-2 program: The stigma around admitting illness has faded, and the Air Force has loosened its rules about permanently grounding sick pilots. The committee on DCS feels confident, however, that the risk has increased, and that the U-2 program needs to change the way it does things.
Henry says he first really understood what had happened to him when his wife sent him a Federal Aviation Administration brochure on DCS she’d found on the Internet shortly after his first severe incident. He says that his training lacked much of the basic information in the circular. He also thinks the Air Force needs to protect pilots by addressing the tempo of operations.
“We all love doing what we do,” says Henry. “But I do think that it’s senior leadership’s job to be more conservative. It’s our job to push hard, as the warrior. And then senior leadership needs to be there to pull back and go, ‘Okay, appreciate the effort, but I want [you] to be safe.’ ” He also points out that there are only 33 U-2s in the Air Force fleet (NASA has two more), so the service can’t afford to crash any.
Smith is more forgiving of the U-2 program’s slowness to react. “I think the Air Force—as well as they understood the problem, as well as medical people could explain it to them—I think they tried to keep us safe,” he says. “It’s just, you know, things don’t move that quickly in the Air Force.”
The Air Force is now taking a number of steps to mitigate the risk to its U-2 pilots, partly as a result of Jersey’s study, according to Lieutenant Colonel Tadd Sholtis, deputy director of public affairs at Air Combat Command. The service is more thoroughly tracking DCS incidents, which will enable further studies to better isolate its causes. U-2 pilots are also performing enhanced pre-breathing, which includes exercise, a practice already common in the astronaut corps. Most important, plans are under way to modify the cockpit’s pressurization from the current 29,000-foot altitude equivalent to a much more comfortable 15,000-foot equivalent.
It will likely be several years before the Air Force knows whether the recent steps are helping. In the meantime, the war in Afghanistan continues to demand frequent, high-altitude flights by U-2 pilots.
For a few years it looked like the Air Force had an alternative to the U-2 that could render the DCS problem moot. The Northrop Grumman Global Hawk, an unmanned, remotely piloted drone, can fly almost as high, and do almost everything a U-2 can do. But this January the Pentagon announced it was cutting a variant of the Air Force’s Global Hawk program, Block 30, that had the same capabilities as the U-2 but was not sufficiently cheaper to fly and maintain. With their retrofitted cockpits, the U-2 should be ready for many years of service.
Things are changing slowly but surely at Beale, and the veteran pilots are telling Jersey they can see a difference in the way the young pilots are being treated and educated about DCS. “A lot of them would have been out of the Air Force and out of a career, kind of like Kevin Henry,” says Jersey. While they may not be able to return to the U-2 cockpit, many pilots who have suffered severe DCS are now flying lower in other aircraft.
Henry retired shortly after being grounded. These days, he trains U-2 pilots at Beale as a contractor, running them through the simulators and showing them how to operate, among other things, the autopilot. The Crew Resource Management department even put together an animation of his near-death experience to show rookies just how dangerous DCS can be. Despite the changes being made to the U-2 program to protect its pilots, Henry points out that pilots are still flying very long missions at 70,000 feet. He’s skeptical of claims that they are safer now than they were in 2006. He hands out copies of the FAA brochure to all his students, just in case.
Mark Betancourt is a freelance writer, filmmaker, and radio producer living in Washington, D.C. His last feature was “World War II: The Movie” (Feb./Mar. 2012).