Gonorrhea Is Developing Antibiotic Resistance
And public health officials are scared of what comes next
/https://tf-cmsv2-smithsonianmag-media.s3.amazonaws.com/filer/69/14/691448ae-14ee-4521-aa24-515d69ee80fd/42-38853151.jpg)
Gonorrhea is preventable and—since the introduction of antibiotics in the 1940s—curable. But the “curable” part could be about to change: As The Guardian’s Ben Quinn reports, antibiotic resistance in some strains of gonorrhea have public health officials in Britain worried that it could become untreatable.
Quinn writes that Sally Davies, Britain’s chief medical officer, has contacted all physicians and pharmacists in England to make sure they are prescribing the right medications to fight strains of the disease that have rapidly developed resistance to commonly used antibiotic treatments. Earlier this year, a study found that up to 20 percent of English physicians were still prescribing out-of-date treatments that do not reflect the latest research on antibiotic resistance in gonorrhea.
Davies’ action is just the latest response to a sequence of events that has spooked health officials. Both the World Health Organization and the Centers for Disease Control and Prevention have sounded the alarm on drug-resistant gonorrhea in recent years.
Earlier this year, an outbreak of so-called “super gonorrhea” in England proved resistant to azithromycin, an antibiotic that is usually administered alongside another antibiotic from the cephalosporin family. In recent years, public health officials have used a combination of two antibiotics to up the chances of the disease responding to one or the other antibiotic. The English outbreak triggered a national alert and brought attention to the illness, which affects an estimated 106 million people worldwide each year. Symptoms include painful urination, discharge, or unexplained bleeding. However, many gonorrhea patients do not exhibit any symptoms at all, making the illness as hard to diagnose as to treat.
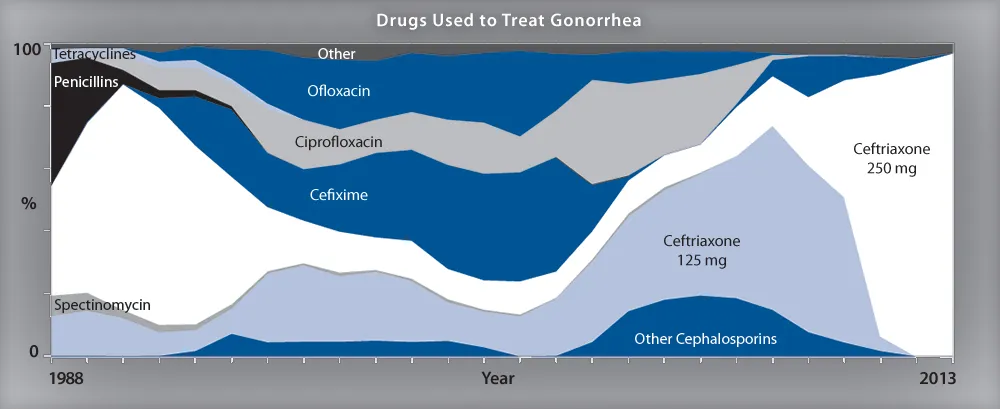
The more drugs gonorrhea resists, the harder the infection will be to treat. Since 1986, the CDC has monitored the resistance of Neisseria gonorrhoeae, the bacteria that causes gonorrhea, to a number of antibiotics. Since then, reports the agency, the bacterium has “developed resistance to nearly all of the antibiotics used for gonorrhea treatment.”
As the public consumes antibiotics, they inadvertently foster more resilient bacteria, so the only choice is for scientists to discover another effective antibiotic combination, a new treatment of some other kind, or an entire new class of antibiotics. The health consequences of untreated gonorrhea—infertility, long-term pain, and permanent arthritis—mean that it’s even more important for public health officials to monitor the disease as it evolves.
There is good news, however. The spread of gonorrhea is preventable. Condom use and abstinence from sex with infected individuals can prevent the spread of the disease, and cases in the United States have dropped from nearly 500 people per 100,000 in the 1970s to about 110 people per 100,000 today. Perhaps with increased vigilance, safer sex and scientific progress, the disease can become even less common in the coming years.
/https://tf-cmsv2-smithsonianmag-media.s3.amazonaws.com/accounts/headshot/erin.png)
/https://tf-cmsv2-smithsonianmag-media.s3.amazonaws.com/accounts/headshot/erin.png)