Ear Tubes May Finally Get an Upgrade
Harvard researchers have invented a new device that might mean fewer visits to the surgeon for kids with chronic ear infections
/https://tf-cmsv2-smithsonianmag-media.s3.amazonaws.com/filer/64/46/64469c3e-068d-4fdb-920c-20862c0b4921/ear_infection.jpg)
At Massachusetts Eye and Ear, a Harvard teaching hospital in Boston, Nicole Black and her classmates were told to look inside each other’s ears using an otoscope to illuminate their eardrums. Black’s peers noticed that she had scar tissue in her ear canal and the instructors suggested the scarring may have been caused by ear tubes that were surgically inserted during her childhood to treat recurring ear infections.
Because Black was a toddler at the time, she doesn’t exactly remember what her own experience was like with ear tubes, which are tiny cylinders inserted into the eardrum to keep the ear properly ventilated and prevent painful clogging. But still, they left a lasting mark, and one day, this scar tissue could lead to hearing loss. Around the time of this class exercise, Black’s nephew underwent ear tube surgery. In fact, several other team members also had loved ones who were getting tubes implanted. With her nephew in mind, Black was motivated to look for a solution, so that perhaps in the future, getting ear infections at a young age won’t have to impact a person for an entire life.
Black, a Harvard University bioengineering PhD candidate, had been working with surgeons at Massachusetts Eye and Ear, Aaron Remenschneider and Elliott Kozin, on other middle ear devices. After deciding to investigate ways to improve ear tubes, they teamed up with materials science researchers from Harvard to create PionEar—a tiny bio-inspired, 3D-printed ear tube that reduces scarring as well as the need for repeated insertion surgery.
Black and her nephew aren’t anomalies: an estimated 80 percent of kids will have at least one ear infection by the time they’re three years old, and these infections account for at least 25 million doctor’s visits annually. Most infections can be treated with antibiotics—either orally or via ear drops. But oral antibiotics used for the whole range of bacterial infections children encounter have been found to have a host of side effects, accounting for nearly 70,000 emergency room visits per year, and are often overused. The Centers for Disease Control and Prevention estimate that 30 percent of all antibiotics prescribed in clinics, doctor’s offices and ERs are unnecessary. Ear drops can be effective, but for cases with complications or ears that are especially clogged, actually getting the drops to the middle ear is a challenge. Nearly 700,000 kids under the age of 15, who are prone to ear infections that come back again and again, are treated in the United States each year with surgically-implanted ear tubes, according to the American Academy of Otolaryngology—Head and Neck Surgery.
However, ear tubes aren’t a foolproof solution either. Ultimately, their purpose is to ventilate the ear in order to reduce pain, not to actually treat the infection. Historically, ear tubes were created by doctors—not engineers or physicists—presumably in a pinch to provide their patients relief. The first ear tube was created in 1845 by German scientists Gustav Lincke and Martell Frank, and about a half dozen models were introduced by 1875 using different materials, including gold, silver, aluminum and rubber. In the 1950s, Beverly Armstrong introduced the first notched vinyl-based tube that is still the basis of what’s used today. There’s been little change to the original design.
Black and the team found that when doctors prescribe ear drops to patients with ear tubes, oftentimes the drops don’t actually reach the middle ear with the tubes in either, and instead, end up pooling at the surface of the tube. What’s more, the tubes often fall out too soon, which sends kids back to the hospital for another operation, which can get invasive, expensive and exhausting.
“We found that almost 40 percent of ear tubes end up failing one way or another,” says Black, who is also pursuing a minor in speech and hearing bioscience and technology. “So these kids end up going back to the operating room. This is especially concerning for me knowing that my nephew could face this.”
Finding a solution that expedites the healing process rather than prolonging it is vital, especially for young kids who are developing language. When ear infections are really bad and mucus is built-up in the middle ear, kids “basically hear like they’re underwater,” says Black. If they can’t hear their own voice or their parents, this can have a huge impact on speech development.
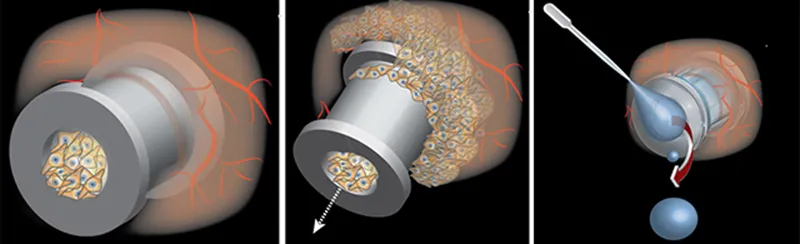
PionEar addresses these issues in several ways. First and foremost, PionEar is smaller than a traditional ear tube and fits snugly in the middle ear in order to reduce scarring and the risk of them falling out early. Secondly, the device reduces the chance of bacterial infection and additional clogging. Lastly, the geometry of PionEar ear tubes allow mucus build-up to drain out of the ear and medicine to flow into the middle ear and effectively treat an infection.
“A key component of the novelty of this invention is the combination of these effects in a single device, which is quite challenging,” says Michael Kreder, a PionEar co-inventor and an applied physics PhD candidate who works in Harvard professor Joanna Aizenberg’s biomechanics lab.
To achieve that second goal, the team drew inspiration from the carnivorous tropical pitcher plants from the Nepenthaceae family, most of which are known for their distinctive champagne flute-like shape. Tiny porous nanostructures within the cup-shaped leaf of most pitcher plants trap moisture and lubricate the rim of the “cup,” so that once a tasty insect lands on the plant, it gets sent down a slip-and-slide to its death in a pit at the base of the plant filled with digestive enzymes.
Riffing off of pitcher plants, Kreder and his colleagues masked the PionEar’s underlying solid material with a liquid layer. This construction ultimately helps prevent bacterial films from forming on the ear tube and causing persistent infection.
PionEar recently won top honors at the Collegiate Inventors Competition, receiving the gold award worth $10,000. The National Inventors Hall of Fame puts on the competition in partnership with the United States Patent and Trademark Office. (The USPTO partners with Smithsonian.com to support stories on innovation at the Smithsonian Institution and beyond.) The team has filed for a provisional patent.

One of the judges of this year’s competition, biomedical engineer Frances Ligler of North Carolina State University, who is best known for her work with biosensors, notes that PionEar is especially exciting due to how its vast potential reach.
“PionEar has the potential to improve hearing in kids more safely at a critical time in their speech development, reduce the pain and cost of repetitive surgeries, and significantly reduce scarring of the eardrum with associated permanent hearing loss,” Ligler says.
Ligler hopes to see PionEar move quickly through the next phases of commercialization, including patent approval, FDA approval of their materials, animal tests and clinical trials. “The sooner the better,” she says.
Black says the team will continue to improve the device’s design using 3D printing methods in Harvard professor Jennifer Lewis' bioengineering lab. Soon, they’ll move toward testing their ear tubes in otolaryngology’s star lab animal, the chinchilla, which—thanks to the rodent’s large ears and similar susceptibility to ear infections—has been instrumental in studying diseases of the inner and middle ear in humans for decades. Remenschneider will lead the animal study at the Massachusetts Eye & Ear hospital. Commercialization efforts are underway with the Wyss Institute for Biologically Inspired Engineering under the guidance of Ida Pavlichenko, a technology development researcher in Aizenberg's lab who is also an instrumental co-inventor of the bio-inspired aspects of PionEar.
“The two inventors explored their solution to a problem that results in widespread suffering, especially of children, from many facets,” says Ligler. “No one has done anything like this before.”
/https://tf-cmsv2-smithsonianmag-media.s3.amazonaws.com/accounts/headshot/rachael.png)
/https://tf-cmsv2-smithsonianmag-media.s3.amazonaws.com/accounts/headshot/rachael.png)